
What Is Causing Physician Burnout And How Can AI Help

by Lev Krasnovsky
April 11, 2024
Physician burnout is on the rise, with over 50% experiencing it in 2021, largely due to time-consuming Electronic Health Record (EHR) documentation. Nearly 75% of burnt-out physicians cite EHRs as a factor, especially senior physicians without support staff. AI-driven solutions like Abstractive Health offer promise by automating note-writing, easing administrative burdens, and allowing more focus on patient care.
Physician burnout has reached epidemic proportions in recent years, with rising rates reported across various medical specialties. According to a recent JAMA health policy paper, more than 50% of physicians were characterized as being burnt out in 2021 (1). This issue not only affects the well-being of healthcare professionals, but also compromises patient care and the healthcare system at large.
Burnout is characterized by “emotional exhaustion, depersonalization, and a feeling of low personal accomplishment” (2). The reasons implicated in the current rise of physician burnout are manifold, but time-consuming Electronic Health Record (EHR) documentation processes regularly serve as a key factor. Specifically, cross-sectional survey data suggest that nearly 75% of physicians with burnout symptoms identify EHRs as a contributor to their burnout (3), and approximately ⅔ of physicians have concerns about how EHRs influence their work-life balance (4). Focusing on the sub-populations most affected, EHRs appear to contribute especially prominently to burnout among senior physicians and those lacking scribes or other support staff for data entry (5).
Electronic health records were intended to streamline healthcare delivery, improve patient care, and enhance clinical decision-making. While EHR systems offer numerous benefits, they also come with their fair share of challenges, particularly in the realm of documentation. Physicians are often overburdened from performing data entry tasks, structuring documentation to comply with regulatory requirements, and navigating through troves of template-generated notes. This technological strain not only detracts from direct patient interaction, but also contributes to feelings of stress and dissatisfaction among healthcare professionals.
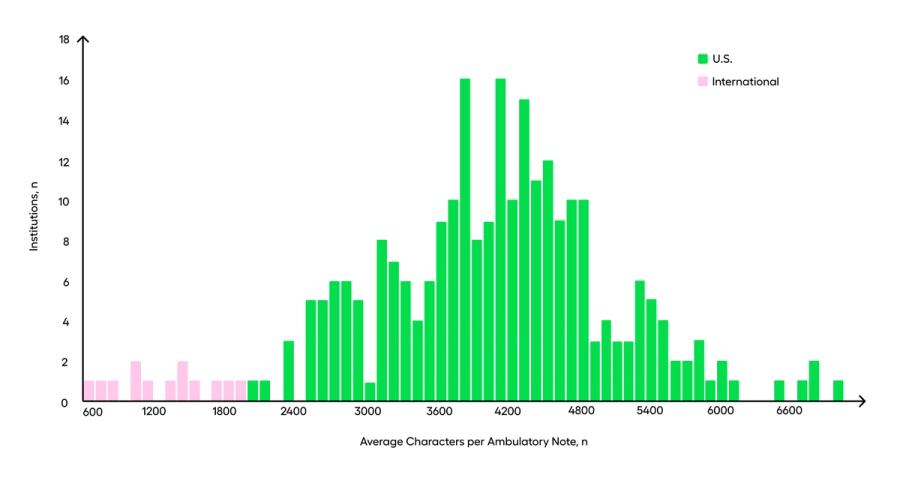
As a 2016 paper published in the Annals of Internal Medicine showed, “For every hour physicians provide direct clinical face time to patients, nearly 2 additional hours is spent on EHR and desk work within the clinic day” (6). The graph below highlights the magnitude of this issue: American medical documentation notes have, on average, nearly 4x as many characters as international documentation (7). The message from these data is not only that a tremendous burden of documentation exists in the US, but that as a consequence, US healthcare professionals must comb through prohibitively-large volumes of documentation to identify data about their patients.
Amidst the challenges of EHR documentation, AI-driven services to streamline clinical note-writing offer a promising solution. Technologies such as Abstractive Health leverage natural language processing algorithms to summarize clinical data and generate comprehensive, contextually-relevant notes. By automating the documentation process, AI-powered systems can significantly reduce the administrative burden on physicians, allowing them to focus more on patient care and clinical decision-making. By embracing AI-driven solutions, we can pave the way towards a healthier, more sustainable future for healthcare professionals.
Related Articles



